If you are considering knee surgery the following total knee replacement information might help you understand the procedure and implants better.
Your knees work hard during your daily routine, and arthritis of the knee or a knee injury can make it hard for you to perform normal tasks. If your injury or arthritis is severe, you may begin experience pain when you’re sitting down or trying to sleep.
Sometimes a Total Knee Replacement is the only option for reducing pain and restoring a normal activity level. If you and your doctor decide a total knee replacement is right for you, the following information will give you an understanding about what to expect. A total knee replacement involves cutting away the damaged bone of the knee joint and replacing it with a prosthesis. This “new joint” prevents the bones from rubbing together and provides a smooth knee joint.

Implant Components
In the total knee replacement procedure, each prosthesis is made up of four parts. The tibial component has two elements and replaces the top of the shin bone or tibia. This prosthesis is made up of a metal tray attached directly to the bone and a plastic spacer that provides the bearing surface.
The femoral component replaces the bottom of the thigh bone or femur. This component also replaces the groove where the patella, or kneecap, sits.
The patellar component replaces the surface of the knee cap, which rubs against the femur. The patella protects the joint, and the resurfaced patellar button will slide smoothly on the front of the joint.
The Procedure
Before you are taken to the operating room you’ll be given medication to help you relax, and the anesthesiologist will talk with you about the medications he’ll be using. In the operating room, you will be placed under full anesthesia.
Returning Home
You will be discharged when you can get out of bed on your own and walk with a walker or crutches, walk up and down three steps, bend your knee 90 degrees and straighten your knee.
At home you should begin ambulation with a cane as tolerated. Keep your incision clean and dry and watch closely for any signs of infection.
You’ll continue your home exercise program and go to outpatient physical therapy, where you will work on an advanced strengthening program and such programs as stationary cycling, walking, and aquatic therapy.
Your long-term rehabilitation goals are a range of motion from 100-120 degrees of knee flexion, mild or no pain with walking or other functional activities, and independence in all activities of daily living.
Once you are “under” the surgeon will begin by making an incision in your leg to allow access to the knee joint. He’ll then expose the joint and place a cutting jig or template on the end of the femur, or thigh bone. This jig allows the surgeon to cut the bone precisely so that the prosthesis fits exactly. Once the femur is cut, the tibia is cut using another jig for proper alignment of the knee prosthesis. The undersurface of the patella is then removed.
Now it’s time to place the prosthesis. This begins with the femoral prosthesis, which is cemented in place using a special bone cement. Next the metal tray is attached to the top of the tibia. This will provide the weight-bearing surface of the femur. The plastic spacer is then attached to the metal tray. This will provide the weight-bearing surface of the femur. If this component should wear out while the rest of the artificial knee is sound, it can be replaced. This is known as a “revision.” Next the patellar button is cemented in place behind the knee cap. Finally, the incision is closed, a drain is put in, and the post-operative bandaging is applied.
Over time, however, a knee replacement may fail for a variety of reasons. When this occurs, your knee can become painful and swollen. It may also feel stiff or unstable, making it difficult to perform your everyday activities.
If your knee replacement fails, your doctor may recommend that you have a second surgery—revision total knee replacement. In this procedure, your doctor removes some or all of the parts of the original prosthesis and replaces them with new ones.
Although both procedures have the same goal—to relieve pain and improve function—revision surgery is different than primary total knee replacement. It is a longer, more complex procedure that requires extensive planning, and specialized implants and tools to achieve a good result.
When Revision Total Knee Replacement Is Recommended
Implant Loosening and Wear
In order for a total knee replacement to function properly, an implant must remain firmly attached to the bone. During the initial surgery, it was either cemented into position or bone was expected to grow into the surface of the implant. In either case, the implant was firmly fixed. Over time, however, an implant may loosen from the underlying bone, causing the knee to become painful.

The cause of loosening is not always clear, but high-impact activities, excessive body weight, and wear of the plastic spacer between the two metal components of the implant are all factors that may contribute. Also, patients who are younger when they undergo the initial knee replacement may “outlive” the life expectancy of their artificial knee. For these patients, there is a higher long-term risk that revision surgery will be needed due to loosening or wear.
Infection
Infection is a potential complication in any surgical procedure, including total knee replacement. Infection may occur while you are in the hospital or after you go home. It may even occur years later.

If an artificial joint becomes infected, it may become stiff and painful. The implant may begin to lose its attachment to the bone. Even if the implant remains properly fixed to the bone, pain, swelling, and drainage from the infection may make revision surgery necessary.
Revision for infection can be done in one of two ways, depending on the type of bacteria, how long the infection has been present, the degree of infection, and patient preferences.
- Debridement. In some cases, the bacteria can be washed out, the plastic spacer can be exchanged, and the metal implants can be left in place.
- Staged surgery. In other cases, the implant must be completely removed. If the implant is removed to treat the infection, your doctor will perform the revision in two separate surgeries. In the first surgery, he or she will remove the implant and place a temporary cement spacer in your knee. This spacer is treated with antibiotics to fight the infection and will remain in your knee for several weeks. During this time, you will also receive intravenous antibiotics. When the infection has been cleared, your doctor will perform a second surgery to remove the antibiotic spacer and insert a new prosthesis. In general, removing the implant leads to a higher chance of curing the infection, but is associated with a longer recovery.
Instability
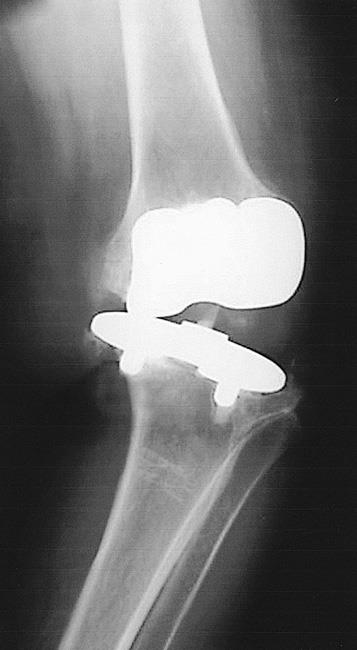
If the ligaments around your knee become damaged or improperly balanced, your knee may become unstable. Because most implants are designed to work with the patient’s existing ligaments, any changes in those ligaments may prevent an implant from working properly. You may experience recurrent swelling and the sense that your knee is “giving way.” If knee instability cannot be treated through nonsurgical means such as bracing and physical therapy, revision surgery may be needed.
Stiffness
Sometimes a total knee replacement may not help you achieve the range of motion that is needed to perform everyday activities. This may happen if excessive scar tissue has built up around the knee joint. If this occurs, your doctor may attempt “manipulation under anesthesia.”

In this procedure, you are given anesthesia so that you do not feel pain. The doctor then aggressively bends your knee in an attempt to break down the scar tissue. In most cases, this procedure is successful in improving range of motion. Sometimes, however, the knee remains stiff. If extensive scar tissue or the position of the components in your knee is limiting your range of motion, revision surgery may be needed.
Fractures
A periprosthetic fracture is a broken bone that occurs around the components of a total knee replacement. These fractures are most often the result of a fall, and usually, require revision surgery.
In determining the extent of the revision needed, your doctor will consider several factors, including the quality of the remaining bone, the type and location of the fracture, and whether the implant is loose. When the bone is shattered or weakened from osteoporosis, the damaged section of bone may need to be completely replaced with a larger revision component.
